Fundus Photography
Fundus photographs are images of the back of the eye. You have probably seen them before: those round, orangey-red pictures hanging in your eye care practitioner’s office with dark and bright spots and branching blood vessels. Your doctor may take fundus photographs of your eye to make sure your optic nerve, vitreous (the gel that fills the eye), retina, macula (center of the retina) and blood vessels are healthy.
First, your pupils will be dilated with eye drops. Then you will look into the special fundus camera. You’ll see a series of bright flashes as the camera takes highly magnified and detailed images of your eye. The whole procedure is painless and takes only 5-10 minutes. The photographs may be compared to earlier images taken of your eyes or filed away for future comparison.
Optomap® Retinal Exam
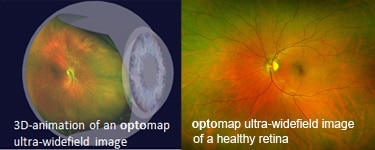
The retina is susceptible to a number of diseases such as macular degeneration, detachment and glaucoma, which can eventually lead to blindness. The Optomap® retinal exam is a noninvasive procedure that quickly and easily takes an image of the retina that your doctor can review for early signs of retinal abnormalities. Early detection of retinal problems can help minimize damage and increase the effectiveness of treatment.
This exam takes an ultra-widefield image of the retina in less than a second without dilating the pupils. The digital image is available on screen immediately for doctor and patient to review together. This evaluation is recommended even if you are not experiencing any eye problems, as many conditions do not cause early symptoms and may otherwise remain unnoticed.
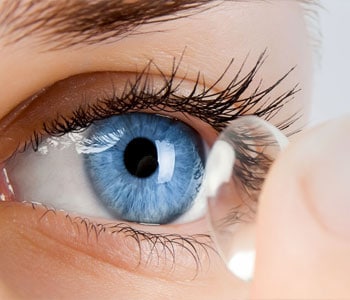
Corneal Topography And Analysis
Corneal topography is a non-invasive medical imaging technique for mapping the “window of the eye”, the cornea. It is a three dimensional topographical map, which evaluates 8,000 to 10,000 specific points across the entire corneal surface. It provides both a quantitative and a qualitative evaluation of the front surface of the cornea.
Corneal topography is invaluable when evaluating Keratoconus and pre- and post-surgical patients, particularly those who have had corneal transplants, radial keratotomy (RK), or LASIK.
When considering contact lens correction for irregular or diseased corneal conditions, corneal topography is absolutely necessary in the ability to manage these complex cases and will thus increase the overall success rate.
Corneal Pachymetry
Corneal Pachymetry is a simple, painless test that is a non-invasive ultrasonic technique for measuring corneal thickness. It has been used primarily in the evaluation for corneal diseases, assessment for patients at risk for glaucoma, and to determine if the patient’s cornea is suitable for any laser vision surgery.
Ultrasonic corneal pachymetry is performed by placing a probe on the central cornea, after a topical anesthetic (numbing) eye drop is administered.
Pachymetry should be done if you are considering LASIK, to ensure that the cornea is thick enough to support the corneal flap. If the cornea is too thin for LASIK, one may be able to use other alternate laser vision correction procedures.
Dry Eye Analysis/ Meibography
Non-InvasiveTear film break-up time (NIKBUT) measures tear film stability and how long a person's tears last. This is measured within seconds.
Images of the health of the meibomian glands is easily and efficiently analyzed. These glands are responsible for the lipid or oil layer of tear fildm Meibomian Gland dysfunction is the most grequesnt cause of dry eye syndrome.